
The Myanmar Eye Care Project was inititiated in 2002 when a Myanmar refugee family, who had settled in Sydney, had inherited the sum of $5000. They asked Geoff to develop an eye care facility at the Village Monastery Hospital of their Chief Abbot, Sayadaw U Lakkhana in Wachet, a small village one hour from Mandalay. The service rapidly burgeoned into a busy clinic and teaching centre supported by the MECP.
Once qualified, Geoff pursued his goals and commenced his life work:
 BOPHUTHATSWANA Between 1982 – 1984 Geoff developed his first project in The Republic of Bophuthatswana, Southern Africa, where he was the sole ophthalmologist.
BOPHUTHATSWANA Between 1982 – 1984 Geoff developed his first project in The Republic of Bophuthatswana, Southern Africa, where he was the sole ophthalmologist.
. For each of nine provinces, he trained a suitable auxiliary group drawn from a nursing background. The delivery of services to a far larger population than he could have covered alone became active. The success of the program persuaded the government to sanction a higher level of responsibility to this new class of professionals.
Doctors oversaw these dedicated teams in carrying out assessments, prescribing glasses and treatments, and performing simple surgical procedures. This strategy met the needs of 42,000 needy individuals within its first twelve months.

Some of the team members.

Screening for glaucoma

Tomorrow he will not need the white stick.
 AUSTRALIA While serving outback communities, Geoff was exposed to and increased his understanding of the field of eyesight restoration, meeting here a profoundly different and challenging pattern of needs
AUSTRALIA While serving outback communities, Geoff was exposed to and increased his understanding of the field of eyesight restoration, meeting here a profoundly different and challenging pattern of needs

After a Corroboree, trachoma screening near Katherine
 INDONESIA Indonesian government data estimated the cataract blindness figure alone to be three million individuals, a backlog of possibly six million operations! Most disturbing and sadly valid, was that 10% of this alarming number was under twenty years of age. Blind children! – a wrenching statistic.
INDONESIA Indonesian government data estimated the cataract blindness figure alone to be three million individuals, a backlog of possibly six million operations! Most disturbing and sadly valid, was that 10% of this alarming number was under twenty years of age. Blind children! – a wrenching statistic.
Commencing in 1988, Geoff established eye care services in Indonesia and devised an intervention to take the eye service to the villages. He teamed up with the dynamic and charismatic John Fawcett and Rotary of West Australia, which had committed to rendering Australia’s beloved holiday island of Bali a cataract-free zone. Rotary International supported this plan by providing a mobile operating theatre.
Sociologic studies had shown that in the Balinese karmic perception, blindness was not a problem. ‘White hair, white eyes’ was the sort of fatalistic aphorism that made people accept the incapacity. Their extended families were less enthused, as they would, with love, take responsibility for the blind person and their family, but maintained awareness that even in one of Indonesia’s wealthy provinces, sufficiency was the rule. Extending the ‘adequate provision’ responsibility of a family was not easy or comfortable.
The families of the blind needed an advocate, so the Australian helpers assumed that role.
The secondary agenda was no less critical: To demonstrate that community-based and affordable eye care is possible. Towards this end, the project trained local doctors in modern microsurgery and lens implantation.
Now known as The John Fawcett Foundation or Yayasan Kemanusiaan Indonesia, its sight-restoring activities have extended from Bali to East Java, Kalimantan, Lombok, and the Eastern Islands and West Papua.

Geoff teaching with Professor Ron Rose of Yale at the Bali bus mobile eye clinic

John Fawcett and Geoff examine a lady on the lumbung at the project office

A boy aged six sees for the first time after cataract surgery
 PAPUA NEW GUINEA In 1993 the PNG Church Medical Council invited Geoff to develop a strategy for eye care in Papua New Guinea. The project entailed teaching eye care to trainee eye surgeons and their nurses and support staff and equipping their systems.
PAPUA NEW GUINEA In 1993 the PNG Church Medical Council invited Geoff to develop a strategy for eye care in Papua New Guinea. The project entailed teaching eye care to trainee eye surgeons and their nurses and support staff and equipping their systems.

The team with nurse Barbara Roberts
and Dr Gavin Stringfellow in Rabaul,
PNG, supporting Dr Jambi Garap-e

A colourful wake on the St. George Channel Islands off PNG

Goroka University students invited Geoff to a ‘Sing-Sing’ where he meets the Asaro Mudmen and tries their headdress
 CAMBODIA The time of the Cambodian emergency was a dark one. The Khmer Rouge had almost comprehensively destroyed education and infrastructure. Doctors and nurses had been fast-tracked through their training because of the desperate need for expertise. In 1998, HelpAge International invited Geoff to teach surgery in Cambodia to its Basic Eye Doctor trainees. The Australian team offered advanced training over the years 1998 – 1999 to six inspired and enthusiastic Cambodian Basic Eye Doctors and their support teams.
CAMBODIA The time of the Cambodian emergency was a dark one. The Khmer Rouge had almost comprehensively destroyed education and infrastructure. Doctors and nurses had been fast-tracked through their training because of the desperate need for expertise. In 1998, HelpAge International invited Geoff to teach surgery in Cambodia to its Basic Eye Doctor trainees. The Australian team offered advanced training over the years 1998 – 1999 to six inspired and enthusiastic Cambodian Basic Eye Doctors and their support teams.
Ek Sarou founded Battambang Ophthalmic Care, where he and his trainees perform surgery on more than a quarter of the entire cataract load of Cambodia.
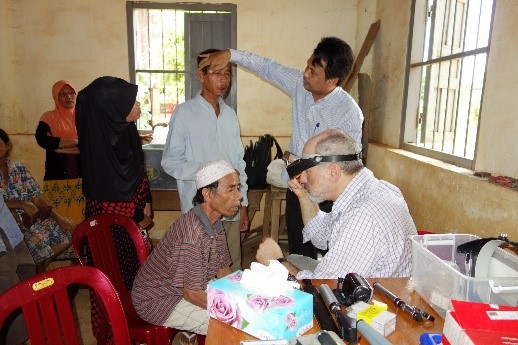
Ek Sarou, Founder of Battambang Ophthalmic Care (BOC), and Geoff screen patients at a Cham Village in South-eastern Cambodia

Geoff with happy BOC patients, celebrating their free sight restoration
 MYANMAR Many Australian, American, Indian and English eye surgeons and nurses have taught at Wachet.
MYANMAR Many Australian, American, Indian and English eye surgeons and nurses have taught at Wachet.
Between 2002 and 2021 the Myanmar eyecare project has developed fourteen eyecare clinics. Four operate independently, and six require only funding support.
Our dream of servicing the impoverished, arid zone of Myanmar was realised in 2013 at the tiny bus junction of Tizaung, which is now a thriving village surrounding a busy eye hospital. Here, our extraordinary coordinator, Daw Phyu Sinn Mon, works with a highly respected monk, Sayadaw U Wunthe Pala Linkara, and the eye team to deliver free sight restoration for the needy on a vast scale.

The staff and students join Sayadaw U Wunthe Pala Linkara and Phyu Sinn Mon to welcome Geoff their teacher

At Mount Popa Taung Kalat, a number of painful trachoma eyelids were repaired on the dining room table
 LADAKH
LADAKH
This remote Buddhist enclave is that part of Tibet that falls within the borders of India. Dr Wangchuk was the sole eye surgeon for a vast and widespread population. No support. He would clean and sterilise his surgical instruments, give a local anaesthetic, bring the patient into the operating room, drape, scrub, operate, return the patient to the ward and start all over.
Efficiency could hardly have been easier to introduce. Train a team of ophthalmic technicians who will screen the towns and villages, supply more operating instruments and an auxiliary who can prepare them so that his expedited role is diagnosis and surgery. A local NGO will maintain support.
Dr Richard Rawson and Optometrist Dean Psarakis joined in the second month of training in the high Himalayas.
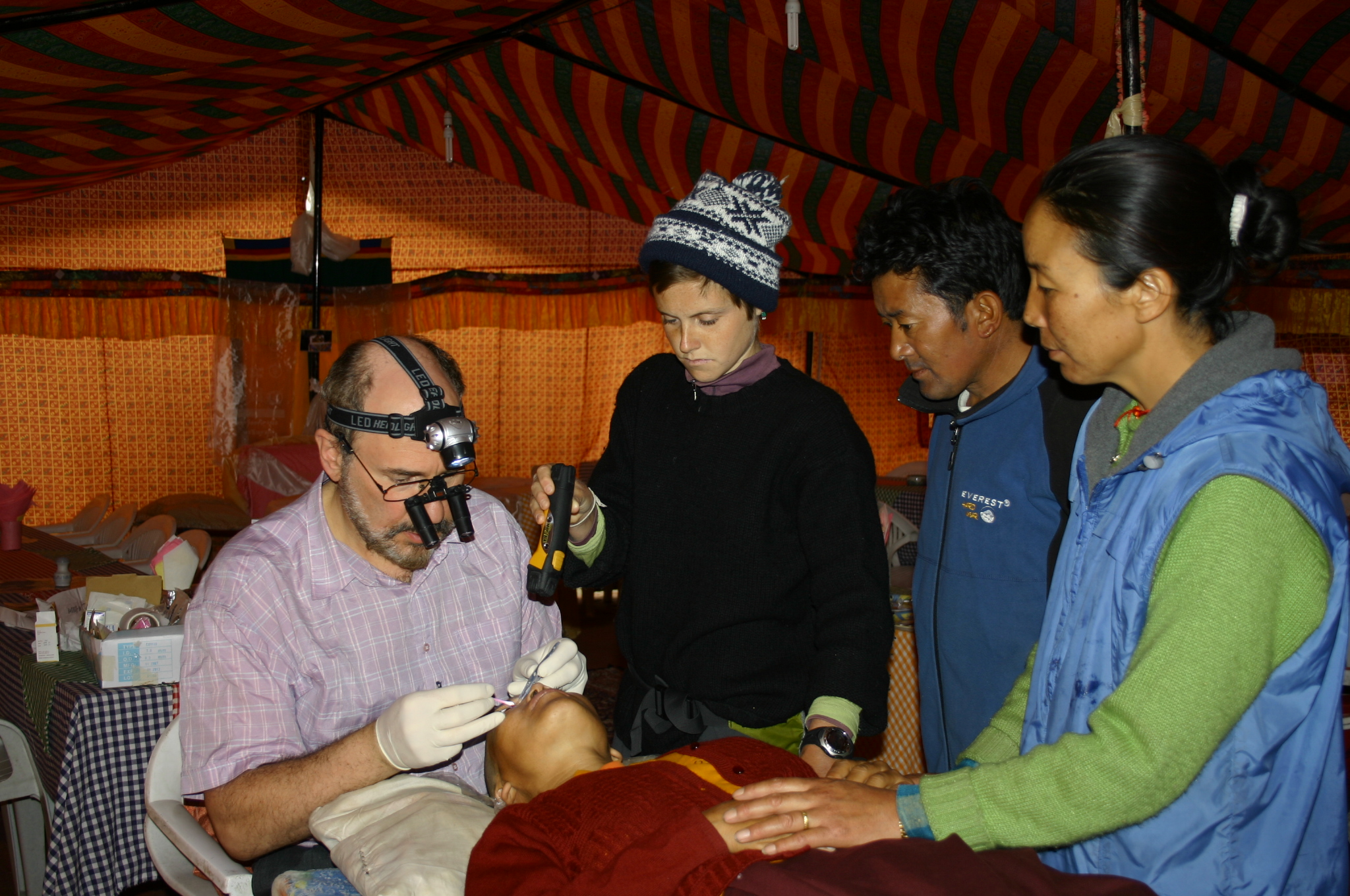
Surgery at high altitude on a dining room table

Young girl after removal of a foreign body

Ladakhi trainees learning refraction
 BIHAR
BIHAR
Geoff responded to a request for help from a remote mission hospital in Southwest Bihar. A superb trainee doctor took little time to master the techniques of eye surgery. Armed with the equipment, Dr Srijit was ready to provide a new service to an impoverished rural community.

Awaiting vision restoration after fifteen years of blindness
Bihari surgeon, Dr Srijit learns cataract surgery

A blind mother sees her child for the first time
 ANDHRA PRADESH
ANDHRA PRADESH
Dr Sunil Thangaraj committed himself to serving a disadvantaged population in rural Andhra Pradesh. Over the years, his breakthroughs have included restoring sight for children previously committed to ‘Blind Schools’, introducing an accredited eye bank to address the prevalent corneal blindness and teaching junior colleagues who come to work with him for upskilling, thus gaining both knowledge and surgical expertise.
Dr Thangaraj has also lens his exceptional expertise many times over the years to the training program in Myanmar.

These village ladies were screened and travelled only 12 km to hospital for treatment

Screening 2000 of the 100 employees of a factory
A young man rescued from the blind school by Dr Sunil (on left). Now sighted, he is training to be a teacher.
 IRIAN JAYA
IRIAN JAYA
The Melanesian population of this eastern outpost of the archipelago has limited access to health care, so Dr Krishnan was willing to extend his surgical skills to include sight restoration. Doctors Geoff Cohn and Stephanie Watson offered the help he needed.
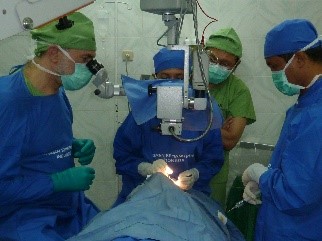
Geoff teaches microsurgery to Dr Krisnan in Timika, West Papua

Exploring Freeport mine after teaching
 BANGLADESH
BANGLADESH
A program in Rangpur, Northern Bangla Desh, needed support. Geoff visited to assess the merits of the service and determine in what ways Australian donors could help. The base is well set up. However, the villages teetering on unstable spits of land, in which they have established feeder clinics, are a bleak prospect—the people certainly stand to benefit profoundly from their service.

Rangpur eye hospital team welcomes Geoff

Operating theatre team at Rangpur
 ETHIOPIA
ETHIOPIA
Dr Lemlem Tamrat gained much from a glaucoma scholarship in Australia. Of most significant promise to her seemed the option of selective laser trabeculoplasty to treat the many glaucoma patients in Addis Ababa and their outreach clinics, people who cannot afford medical or surgical treatment. Geoff delivered and assembled an Australian-made laser in her department’s clinic. It is well used.

Impossibly overcrowded eye clinic
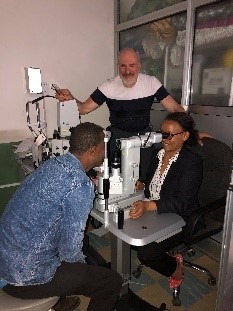
Dr Lemlem Tamrat treats glaucoma with a donated laser delivered by Geoff
 NIGERIA
NIGERIA
Dr Jagun Omodelly had, like Dr Tamrat, discovered the immense value of selective laser trabeculoplasty. Open-angle glaucoma is a scourge in Africa, blinding a large cohort of people, many young and productive with family responsibilities. The COVID-19 pandemic made travel impossible, but See Again International couriered the laser to her in Lagos.
Geoff’s Honours and Acknowledgements
Over the years, Geoff Cohn has accrued many honours for his dedication to restoring eyesight: He was awarded an OAM in 2010. The Power of One Australian Hero’s Award hosted by Penguin Books and The Bryce Courtenay Foundation shortlisted this project. Geoff is a Paul Harris Fellow, and Rotary has granted him life Membership.


